South Africa is renowned for our beautiful climate, picture perfect beaches and bucket-list bushveld adventures. An active outdoor lifestyle together with one of the highest monitored global ultraviolet levels sets the stage for our South African population to have one of the highest skin cancer rates world-wide.
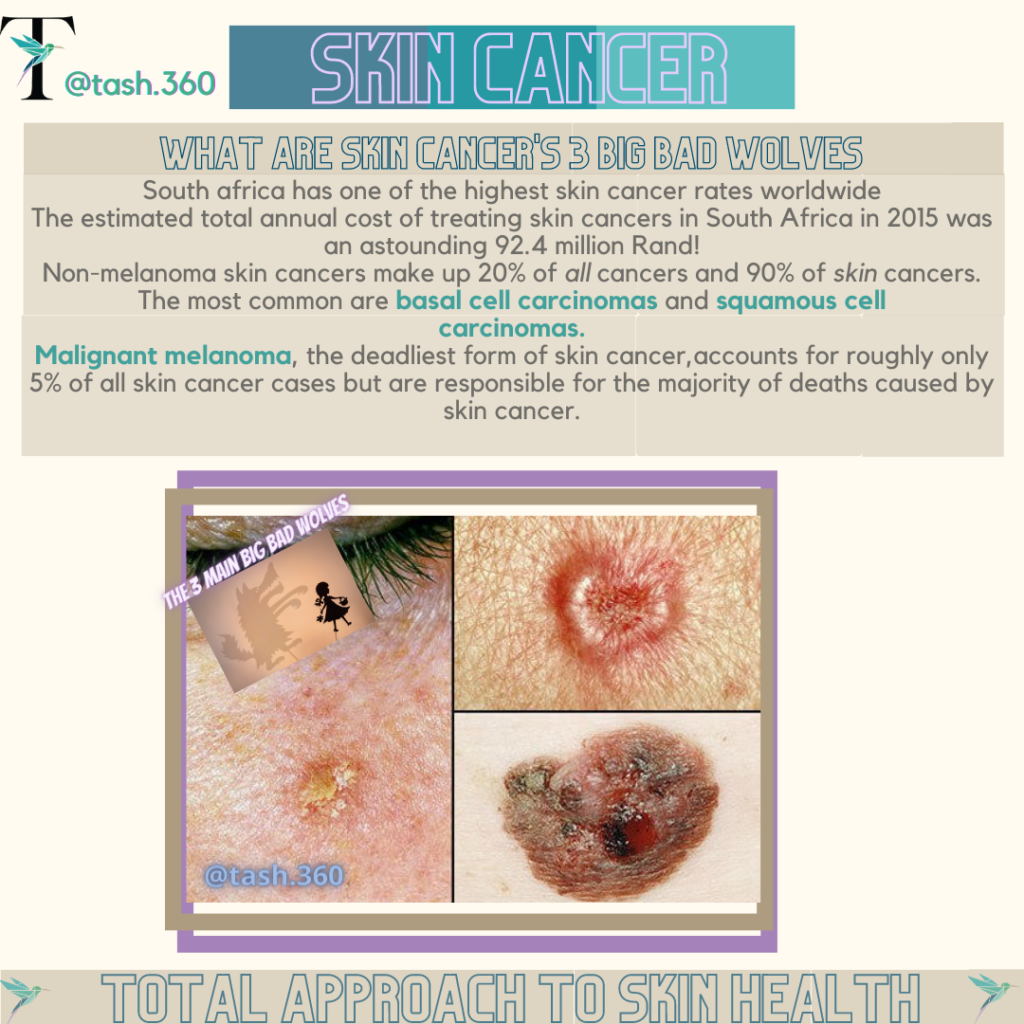
Skin cancer occurs when the DNA in skin cells becomes damaged and is not able to repair itself anymore. This damage causes the skin cells which are affected to start to grow and divide uncontrollably. There are 3 main big bad wolves when it comes to skin cancer:
![]() Big Bad Wolf #1: Basal Cell Carcinoma:
Big Bad Wolf #1: Basal Cell Carcinoma:
Basal cell carcinomas make up about 2/3 of all skin cancers in South Africa and according to the National Cancer Registry in 2013, there were almost 16 000 new cases of basal cell carcinomas reported. These malignancies, sometimes called “rodent ulcers”, thankfully rarely metastasize or kill, but they can still cause significant morbidity through local destruction and disfigurement. They are raised, translucent, pearly nodules that may crust, ulcerate and sometimes bleed. They are found most often on the face and other sun-exposed areas but can appear anywhere. It can involve nerves and even invade into bone.
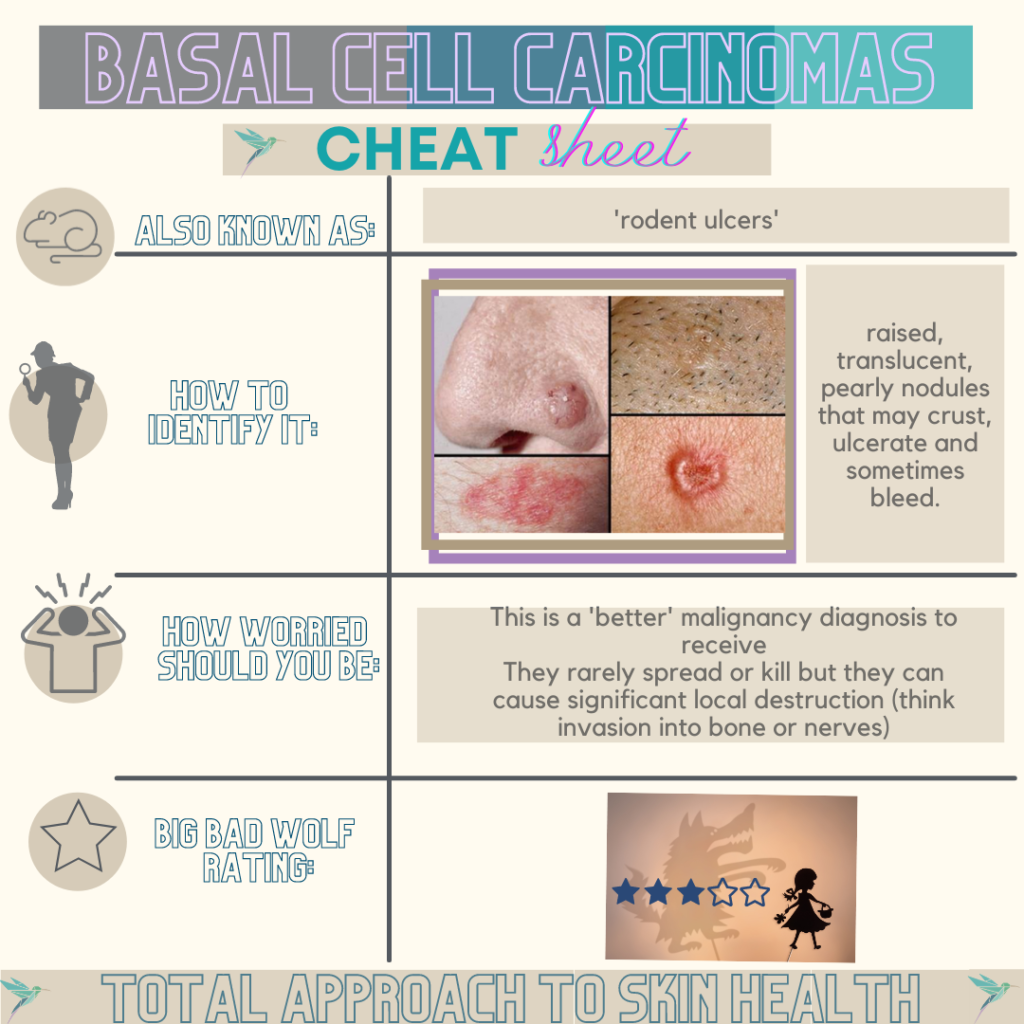
Although considered a “better” diagnosis to receive, it still needs to be treated with respect and dealt with in the earliest possible stages. Basal cell carcinomas can be cured in almost every case, although treatment can be more complicated if the cancer has been neglected for a long time, or if it occurs in an awkward place, such as close to the eye or on the nose or ear.
At TASH360, we will explain the importance of the subtype of basal cell carcinoma with its implications on treatment choice. For example, superficial basal cell carcinomas can be treated with topical creams while nodular basal cell carcinomas are excised. We will carefully weigh up the best and safest course of treatment with the optimal possible cosmetic outcome. Together with you, all variables will be considered and a treatment plan formulated.
![]() Big Bad Wolf #2: Squamous Cell Carcinoma:
Big Bad Wolf #2: Squamous Cell Carcinoma:
Squamous cell carcinomas make up almost 30% of all skin cancers in South Africa and there were 6500 new cases of squamous cell carcinomas reported in 2013 according to the South African National Cancer Registry. These statistics are much higher than the statistics of squamous cell carcinomas globally where they make up a mere 10% of all skin cancers. As they are more aggressive malignancies as compared to basal cell carcinomas, this is a critical fact. They can become disfiguring and sometimes deadly if allowed to grow and carry a 2-6% risk of metastasis. These are not malignancies to mess around with!
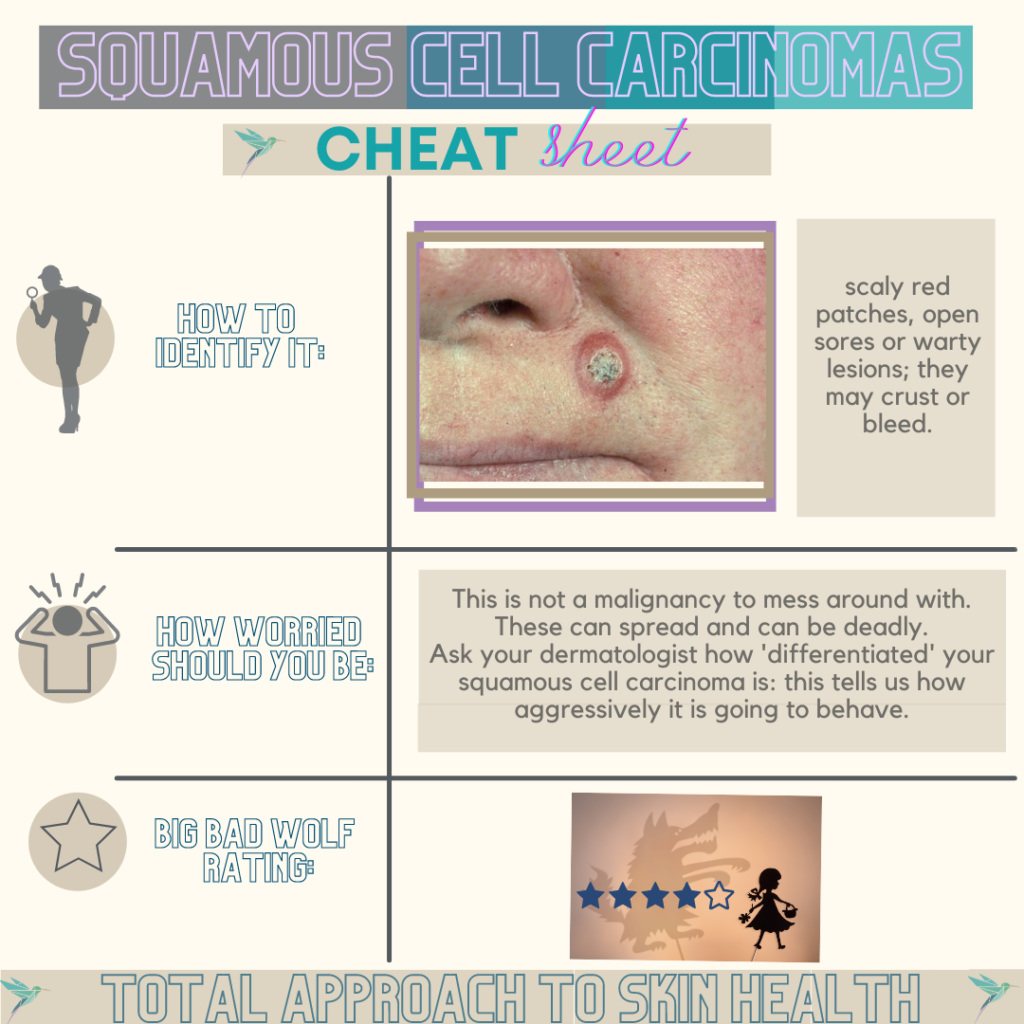
They are most commonly found on sun-exposed areas as UV exposure is the most important risk factor but squamous cell carcinomas can also develop in skin damaged by other forms of radiation, in burns and persistent chronic ulcers, wounds and in old scars. They often look like scaly red patches, open sores or warts; they may crust or bleed. Please visit our experienced team of dermatologists at TASH360 if you have noticed any lesion of concern for immediate attention.
![]() Big Bad Wolf #3: Malignant Melanoma:
Big Bad Wolf #3: Malignant Melanoma:
The South African National Cancer Registry reported 1500 new cases of melanoma in 2013. The diagnosis of a malignant melanoma strikes fear into the heart of a dermatologist because these malignancies can spread rapidly through lymphatics and blood to involve other organs. Melanoma is a type of skin cancer, which arises from the pigment cells (melanocytes) in the skin. In a melanoma skin cancer, the melanocytes become malignant and multiply excessively. One of the most important causes of melanoma is exposure to ultraviolet light. The use of artificial sources of ultraviolet light, such as sunbeds, also increases the risk of getting a melanoma.

Melanocytes make a brown/black pigment (known as melanin), and often the first sign of a melanoma developing is a previous mole changing in colour or a new brown/black lesion developing. Most frequently there is darkening in colour but occasionally there is loss of pigmentation with pale areas or pink areas developing.
At TASH360, we will always address any specific concerns which prompted you to book your appointment, but will urge you to take advantage of our Mole Mapping and skin cancer screening service as well. Melanomas if caught early have a very good prognosis and require only a wide excision. More advanced melanomas unfortunately carry a very poor prognosis. We cannot emphasise enough the value of annual screens and the care we take during the screening process to teach you simple things to watch out for at home.
![]() So what should you be doing?
So what should you be doing?
You should be having at least annual skin cancer screenings. This is a visual inspection of your entire body for suspicious growths, moles or lesions. A complete head-to-toe examination will be done even taking note of the webspaces of the toes and parting the hair to take a good look at the scalp! Your dermatologist will use a dermatoscope, a hand-held device that enables a deeper look into the skin to aid in the diagnosis of suspicious lesions.

There really is no list of criteria which you need to fulfil in order to qualify for this screening. Along with our beautiful climate comes a good dollop of UV exposure and thus an increased risk of skin pre-malignancies and malignancies. Whether you have had excess sun exposure over time or a few blistering sunburns, this is an annual check which needs to be prioritised. Regular screenings which are completely non-invasive and painless are the best way to catch skin cancer in its earliest stages when it is most treatable. Red flags to visit the practice sooner than scheduled are an irritated flaky patch of skin, a “pimple” which will not heal or which bleeds, a pearly bump laced with tiny blood vessels or a non-healing sore. We encourage pop in visits between scheduled appointments if you notice anything which looks odd or suspicious.
The dermatology team at TASH360 are committed to providing unparalleled care in the screening and treatment of skin malignancies. We discourage the isolated examination of an individual lesion and offer meticulous full body screening so that you leave our practice confident that no lesion has gone unnoticed