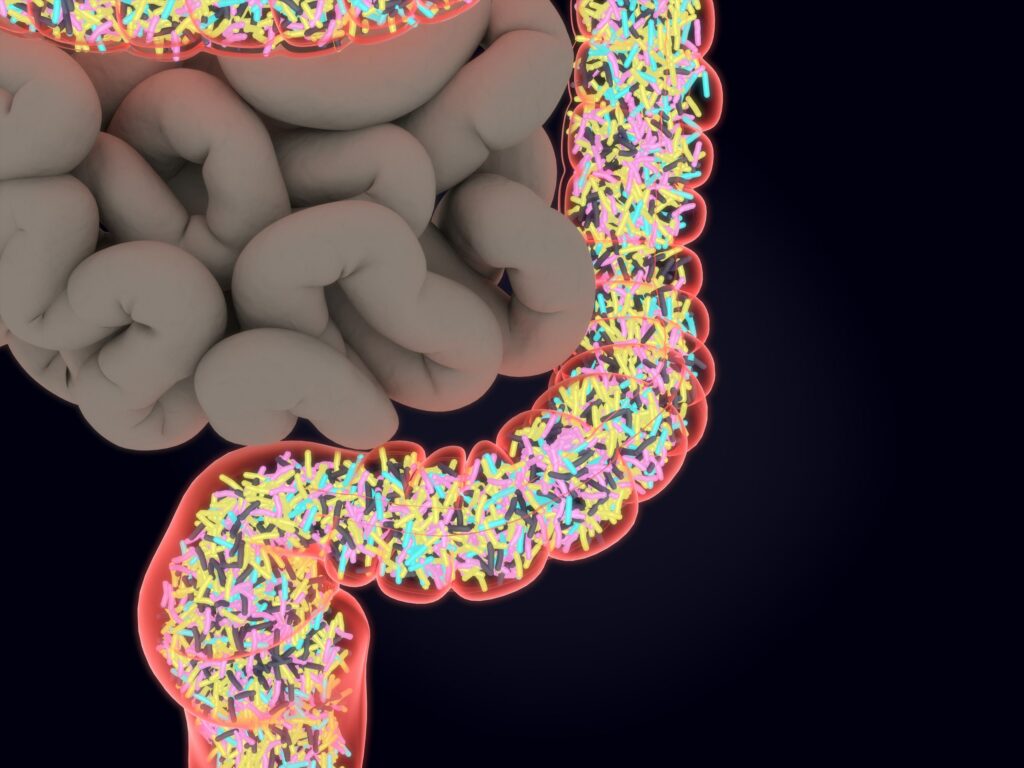
You’ve probably heard a lot about ‘dysbiosis’, otherwise described as an ‘imbalance’ in community of microbes in your gut. Perhaps, you’ve been told that you have too many ‘bad’ bugs & not enough ‘beneficial’ bugs? Or, you’ve been told that you’ve got an ‘overgrowth’ of bugs higher up in the GI tract?
The above may be true for you, however, the science of testing & confirming whether the ‘diagnosis’ is IN FACT true is complex. Your gut microbiome is an active, ever-changing community of living organisms. They’re known to primarily inhabit parts of large intestine, but can move higher up in the gut (hello, SIBO – Small Intestinal Bowel Overgrowth) in response to poor gut motility, chronic constipation, use of certain medications (think PPI’s or antibiotics), psychological stress & anxiety, and an altered release of bile or digestive enzymes.
Basically, a stool test involves a sample taken at a ‘set-point’ in time, and is only ‘picking up’ bugs from the large intestine (for those who didn’t take biology – stool forms in the large intestine), so it doesn’t indicate what’s happening in the upper GI tract (although, SIBO breath testing can be used for this & is now becoming more readily available – thanks scientists!). So, as with many other medical tests, stool testing has its limitations; but that doesn’t negate its power to ‘shed light’ onto what’s really going on inside the gut. Alongside a clinical history, results from a stool test act as a ‘road map’ to assist practitioners to confirm & refine treatment protocols. Now, with that said & understood (hopefully), let’s discover what we can learn from a stool test:
![]() What can you learn from the stool test?
What can you learn from the stool test?

![]() Infections
Infections
Labs can analyse your stool using a microscope, or they can confirm the existence of pathogens by detecting the presence of their genetic material (DNA/ RNA). Pathogens – whether bacterial, parasitic or viral – are more common than you’d think; and not all individuals with positive findings for pathogens will present with common symptoms like stomach cramps, diarrhoea, vomiting or nausea.
![]() Dysbiosis
Dysbiosis
‘Dysbiosis’ is the scientific word that broadly refers to a disruption of the complex gut microbial community. Remember, there are a near infinite number of possible fungi, bacteria and viruses that exist in one’s gut at a set point in time; and all of these ‘bugs’ act together to produce certain compounds that have the potential to influence one’s wellbeing. At present, our exact definition of a ‘healthy’ microbiome is constantly changing as we gather data overtime & as artificial intelligence (AI guys, come on, medicine needs you) meets biology in order to consistently keep tabs of our ‘bugs’ and their metabolites.
At present, stool tests detect the presence of certain good bacteria, and opportunistic (potentially harmful) bacteria & yeasts:
Yeast Overgrowth
At present, stool tests detect the presence of certain good bacteria, and opportunistic (potentially harmful) bacteria Candida albicans is a commonly known fungus, although many more exist. As with anything in life, too much of one thing is never good. An overgrowth of fungi typically occurs after use of antibiotics, and has been associated with symptoms such as bloating, diarrhoea, pruritis, psoriasis, rosacea, acne, and fatigue & ‘foggy brain’.
Opportunistic Bacteria (Bacterial Overgrowth)
This includes a group of bacteria that have the potential to become harmful – otherwise known as being ‘potentially pathogenic’. In small numbers, they’re known to make a part of a ‘normal’ or ‘healthy’ microbiome; however, in large numbers, they’re harmful. We don’t want to allow these bacteria to overgrow!
Beneficial Bacteria & SCFA’s
These are the ‘good guys’, who are often missing. They produce ‘anti-inflammatory’, ‘gut-healing’ messengers known as short-chain fatty acids which keep our immune systems in-check and protect the integrity of the gut lining (protect us against ‘Leaky Gut Syndrome’). These bacteria need to be fed (hello, Fibre) and supported to keep your gut in tip-top condition.
![]() Inflammation
Inflammation
Multiple immune markers can be tested, but here are some that are commonly looked at:
- Calprotectin (a protein released by the immune cells, neutrophils) is a marker that is associated with active inflammation in the gut. The higher the level of calprotectin in the stool, the more inflammation is present in your intestines. If your levels are significantly elevated, then it’s highly likely that you’ll need to be referred to a GI specialist.
- IgA & eosinophil (EPX) levels are useful to gauge what your immune system is doing – whether it’s over- or under-active. Both increase in the presence of ‘bad bugs’, or in response to food allergies. Interestingly, suppressed levels (an ‘under-active’ immune state) of IgA are seen in cases of inadequate nutrition & extreme mental or physical stress. In other words, optimal nutrition & mental health are important for ‘healthy’ immunity.
![]() Leaky Gut
Leaky Gut
In the recent years, scientists have attempted to detect a valid biological marker to test one’s ‘degree’ of ‘leaky gut’. At present, some labs are using two nonmetabolizable sugars, known as lactulose & mannitol, as markers for intestinal permeability & absorptive capacity. Mannitol is a small molecule – it should pass through the gut wall easily in ‘healthy’ individuals who are absorbing well. Whereas, lactulose is larger and should be ‘held back’ from moving through the gut wall in the presence of a well-intact gut lining.
![]() Maldigestion & Malabsorption
Maldigestion & Malabsorption
Digestive Capacity (Pancreatic Elastase)
Maldigestion: Pancreatic elastase levels in stool are used to demonstrate digestive capacity, as it is indicative of the ‘release’ of digestive enzymes (a.k.a little ‘pac-men’ that break down your food) into your gut. If your levels are low, then you may need additional digestive support to ensure that you’re breaking down your food properly.
Malabsorption: We can test for the presence of proteins & fats in your stool (and use the lactulose: mannitol test, as mentioned above) . If high amounts are found, then it’s clear that you’re not absorbing your food effectively.
TAKE HOME MESSAGE
At TASH 360, we use your story, symptoms, and when necessary – lab tests, such as a ‘stool test’ – to confirm whether your gut is ‘leaky’. Gut healing is rarely fast or easy: it’s not as simple as cutting out gluten, adding a forkful of sauerkraut, or including the latest in-supplement into your regimen. It entails a thoughtful, personalized and targeted approach – which always requires your best effort, alongside our expertise.
Get the guidance you need today. We’re by your side.
.